Dermatological Manifestations of Mycoplasma pneumoniae in a 10-Year-Old Boy
A 10-year-old and previously healthy Caucasian male presented with a 2-week history of fever, cough, and pruritic rash. Fever started 2 weeks before presentation, with a maximum temperature of 101.9°F; his fever was low grade on the day of presentation at 100.1°F, without associated chills or rigors.
Ten days before presentation he complained of a sore throat and cough and was empirically treated by an outside facility for streptococcal pharyngitis with amoxicillin. The cough was dry and progressively worse, with no diurnal or postural variation and no chest pain.
 On day 2 of illness, he developed a pruritic rash that started as a single erythematous macule on his abdomen (Figure 1) that spread to his arms and legs, then his face—specifically on his cheeks—and eventually his palms (Figure 2) and soles (Figure 3) by day 8 of illness. The rash on his trunk was pinpoint punctate but not petechial. It was maculopapular, nonconfluent with discrete margins and without umbilication. The patient self-treated with cortisone cream, eucerin, epson salts, and topical antihistamine, with minimal success.
On day 2 of illness, he developed a pruritic rash that started as a single erythematous macule on his abdomen (Figure 1) that spread to his arms and legs, then his face—specifically on his cheeks—and eventually his palms (Figure 2) and soles (Figure 3) by day 8 of illness. The rash on his trunk was pinpoint punctate but not petechial. It was maculopapular, nonconfluent with discrete margins and without umbilication. The patient self-treated with cortisone cream, eucerin, epson salts, and topical antihistamine, with minimal success.
His fever and cough did not improve with the 10 days of amoxicillin. He reported no contact with others who were sick, and his vaccinations were up-to-date. There was a history of travel to Connecticut and North Carolina 2 months before presentation. There was also a history of close contact with chickens, pigeons, and doves. The patient reported no major illness before these symptoms, or relevant family history.
On admission, the patient was febrile and tachypneic but nontoxic appearing. His dermatological exam showed a generalized, pruritic urticaria-like exanthem with raised erythematous plaques on the trunk, palms, and soles. There was no conjunctival or mucosal involvement.

His oropharynx was clear, with some mild pharyngeal erythema without exudate. Auscultation of the lungs was normal, his cardiac exam was benign, and the patient’s abdominal exam was benign without organomegaly.

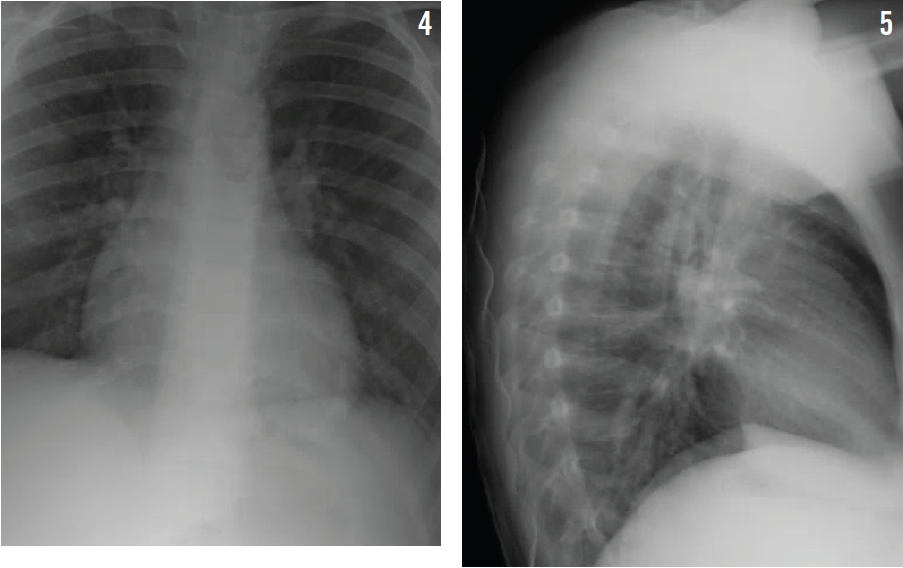
Chest radiography showed patchy areas of consolidation distributed in both lungs, suggesting bronchopneumonia (Figures 4 and 5). Laboratory tests showed: hemoglobin 14 g/dL; total leukocyte count (TLC) 8,300/mm3; neutrophils 85%; and lymphocytes 9%. Testing results for infectious mononucleosis were negative. Results for the patient’s complete metabolic panel were normal. A blood culture showed no growth, and his respiratory viral panel was negative.
Diagnosis: Dermatological Manifestation
Serology for Mycoplasma pneumoniae immunoglobulin (Ig)M was positive at 6380 U/mL (negative is 0 to 769 U/mL). Mycoplasma cold agglutinin (CA) was 1:512 (negative is < 1:32). A number of cutaneous manifestations associated with M pneumoniae as extra pulmonary have been described. The most common of these manifestations is the exanthematous rash or maculopapular rash, with an incidence of 8% to 33%.1 Less frequent but also common include urticaria, erythema nodosum, and Stevens-Johnson syndrome. Fuchs syndrome, a variant of erythema multiforme predominantly involving the mucosal surfaces (erythema, erosions, and ulcerations of the oral or rarely genital mucosa and severe conjunctivitis) with sparing of the skin, may pose a diagnostic challenge and has in the past been found to have M pneumoniae as one of its etiological factors.2
Most of the cutaneous lesions are thought to be due to the host’s immune response to antigens on the microbes, rather than the microbe itself. 3
One-third of acute childhood urticaria leading to hospitalization may be related to M pneumoniae infection, implying that urticaria refractory to antihistamine treatment in the absence of allergens should seek serologic examinations for M pneumoniae.4
Finland et al described the occurrence of CAs in 50% to 70% of patients with M pneumoniae infections.5 CAs are oligoclonal IgM autoantibodies directed against an altered I antigen on the surface of erythrocytes from M pneumoniae–infected patients. CA autoantibodies were used to support the serologic diagnosis of acute M pneumoniae, because they are the first to be detected and to disappear. CA autoantibodies appear within the first 7 to 10 days after infection and persist for 8 to 12 weeks; the titer of these antibodies usually exceeds 1:128 in patients with pneumonia.
Currently, the most sensitive and specific test for the detection of M pneumoniae infection is ELISA, which detects specific IgM antibodies to M pneumoniae.6 Despite the availability of ELISA for IgM, a bedside test for CAs is still the most rapid test available to support the diagnosis of acute M pneumoniae infection. However, mycoplasma IgM still carries a chance for false-positive results, so the gold standard is polymerase chain reaction for detecting the actual mycoplasma antigen.
An awareness of the presentations of M pneumoniae as a cutaneous disease is essential. Cutaneous manifestations could appear at any time during the disease process (ie, before), with or even after the appearance of pulmonary symptoms. Therefore, this accounts for knowledge of and high index of suspicion of mycoplasma infection for early diagnosis and treatment. A chest radiograph alone is not sufficient to make the diagnosis. Serological examinations are recommended, and once the diagnosis of M pneumoniae is confirmed, the treatment of choice is macrolides (azithromycin, clarithromycin).
Conclusions
Cutaneous manifestations are not rare in M pneumoniae. A high index of suspicion is needed when dealing with patients who exhibit skin manifestation with or without respiratory tract symptoms. Serological testing is the gold standard in making the diagnosis. Finally, the treatment of choice comes from the macrolide group of antibiotics, such as azithromycin 10 mg/kg/day the first day, followed by 5 mg/kg for 4 days.
Alireza Habibi, MD, is a resident in the Department of Pediatrics at the University of Nevada School of Medicine in Las Vegas, Nevada.
Gagandeep Singh, MD, is a resident in the Department of Pediatrics at the University of Nevada School of Medicine in Las Vegas, Nevada.
Alvaro Galvis, MD, is a resident in the Department of Pediatrics at the University of Nevada School of Medicine in Las Vegas, Nevada.
Anthony Shoo, MD, is a resident in the Department of Pediatrics at the University of Nevada School of Medicine in Las Vegas, Nevada.
Pisespong Patamasucon, MD, is a pediatric infectious disease specialist and a professor in the Department of Pediatrics at the University of Nevada School of Medicine in Las Vegas, Nevada.
References
- Copps SC, Allen VD, Sueltmann S, Evans AS: A community outbreak of Mycoplasma pneumoniae. JAMA. 1968;204:123-128.
- Havliza K, Jakob A, Rompel R. Erythema multiforme majus (Fuchs syndrome) associated with Mycoplasma pneumoniae infection in two patients. J Dtsch Dermatol Ges. 2009;7:445-448.
- Narita M. Pathogenesis of extrapulmonary manifestations of Mycoplasma pneumoniae infection with special reference to pneumonia. J Infect Chemother. 2010;16:162-169.
- Kano Y, Mitsuyama Y, Hirahara K, Shiohara T. Mycoplasma pneumoniae infection-induced erythema nodosum, anaphylactoid purpura, and acute urticaria in 3 people in a single family. J Am Acad Dermatol. 2007;57(2 suppl):S33-S35.
- Finland M, Peterson OL, Allen HE, et al. Cold agglutinins. I. Occurrence of cold isohaemagglutinins in various conditions. J Clin Invest. 1945;24:451-457.
- Luby JP. Pneumonia caused by Mycoplasma pneumoniae infection. Clin Chest Med. 1991;12:237-244.


